Recent studies suggest a role for sleep and sleep problems in the etiology of attention deficit hyperactivity disorder (ADHD) and a recent model about the working mechanism of sensori-motor rhythm (SMR) neurofeedback, proposed that this intervention normalizes sleep and thus improves ADHD symptoms such as inattention and hyperactivity/impulsivity.
Linda Walker discusses Neurofeedback on WVUA’s “Brain Matters” radio show
Dr. BJ Guenther interviews 2 experts in the field of neurofeedback. Discussion includes definition and uses of neurofeedback for mental health issues such as depression, anxiety, ADHD, etc. Listen here.
Sleep maintenance, spindling excessive beta and impulse control: an RDoC arousal and regulatory systems approach?
View the PDF
“In this study we aimed to investigate the relation between arousal systems (EEG-beta phenotypes also referred to as spindling excessive beta (SEB), beta spindles or sub-vigil beta) and the behavioral dimensions: insomnia, impulsivity/hyperactivity and attention. This analysis is conducted within a large and heterogeneous outpatient psychiatric population, in order to verify if EEG-beta phenotypes are an objective neurophysiological marker for psychopathological properties shared across psychiatric disorders.”
EEG – Lessons From A Half-Million Brains
Listen to the full podcast here Jay Gunkelman Podcast
This week we’re joined by QEEG Diplomate (yes, that’s a term!) and founder of Brain Science International Jay Gunkelman, to talk Electroencephalography. After analyzing over a half-million EEG scans, Jay has a pretty robust set of human brain data at his disposal… And he uses that body of knowledge to guide the work of psychiatric and other health professionals who make proscriptive recommendations about patients’ brains.
Differential effects of theta/beta and SMR neurofeedback in ADHD on sleep onset latency
Pharmaco-EEG: A Study of Individualized Medicine in Clinical Practice
Ronald J. Swatzyna, Gerald P. Kozlowski, and Jay D. Tarnow
Abstract
Pharmaco-electroencephalography (Pharmaco-EEG) studies using clinical EEG and quantitative EEG (qEEG) technologies have existed for more than 4 decades. This is a promising area that could improve psychotropic intervention using neurological data. One of the objectives in our clinical practice has been to collect EEG and quantitative EEG (qEEG) data. In the past 5 years, we have identified a subset of refractory cases (n = 386) found to contain commonalities of a small number of electrophysiological features in the following diagnostic categories: mood, anxiety, autistic spectrum, and attention deficit disorders, Four abnormalities were noted in the majority of medication failure cases and these abnormalities did not appear to significantly align with their diagnoses. Those were the following: encephalopathy, focal slowing, beta spindles, and transient discharges. To analyze the relationship noted, they were tested for association with the assigned diagnoses. Fisher’s exact test and binary logistics regression found very little (6%) association between particular EEG/qEEG abnormalities and diagnoses. Findings from studies of this type suggest that EEG/qEEG provides individualized understanding of pharmacotherapy failures and has the potential to improve medication selection.
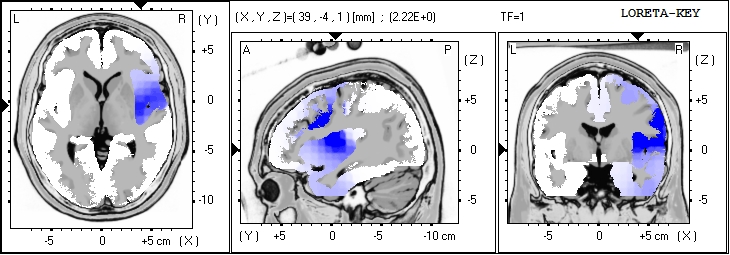
Techniques Effecting the LORETA Source Solution
LORETA can be done in a few ways… as a source analysis for the entire EEG or segment being analyzed… or after a decomposition into the ICA components… The later will provide a better estimate of generators of the
individual components which are all blended for the overall LORETA, distorting the sources with other sources.
Prof. Juri D. Kropotov Interview 2013
Juri speaks about the recent ERP meeting in St Petersburg Russia, held during the summer’s “white nights” when the night sky does not darken fully and the night is very short. Juri is interviewed in his offices, only 200 meters from Pavlov’s famous laboratory.
The discussion of the new methodology of ICA decomposition of the ERP, as well as the benefit of ERP added to the EEG/qEEG is discussed. There is discussion of the diagnostic specificity of the ERP methods, and the concept of biomarkers.
Medication Failure: EEG/qEEG Findings Provide Evidence
This is the PowerPoint “Medication Failure: EEG/qEEG Findings Provide Evidence” as presented at ISNR Conference Workshop 20 September 21, 2013
Presented by:
Ronald J. Swatzyna, Ph.D., L.C.S.W.
The Tarnow Center for Self-Management
drron@tarnowcenter.com
Vijayan K. Pillai, Ph.D.
The University of Texas at Arlington
pillai@uta.edu
FDA Approval of EEG Aid for ADHD
There has been a lot of discussion since the FDA announced approving a new medical device just approved to assist in the diagnosis of ADHD in children and adolescents. “The device, the Neuropsychiatric EEG-Based Assessment Aid (NEBA) System, is based on electroencephalogram technology, which records different kinds of electrical impulses given off by neurons in the brain and the number of times the impulses are given off each second. The NEBA System is a 15- to 20-minute noninvasive test that calculates the ratio of two standard brain-wave frequencies, known as theta and beta waves; the ratio has been shown to be higher in children and adolescents with ADHD than in those without it, according to FDA” (http://alert.psychiatricnews.org/2013/07/ fda-approves-device-to-help-diagnose.html). However, the use of this technology to assist in the diagnosis of ADHD is not new.
David Rabiner, Ph.D. (Senior Research Scientist, Duke University) published a report (Attention Research Update April 2001) titled “New Support for the Use of qEEG scanning in Diagnosing ADHD” (http://www.helpforadd.com/2001/april.htm). This report acknowledged utilizing the measure of the ratio of theta to beta waves in the prefrontal cortex as a marker for ADHD (ages 6-20). Therefore the technology is not new, and although the NEBA System is helping to bring scientific evidence into the realm of psychiatric diagnosis, there is more to it then has been discussed thus far.